Know more about Bacterial Vaginosis/Vaginitis
BACTERIAL VAGINOSIS / VAGINITIS
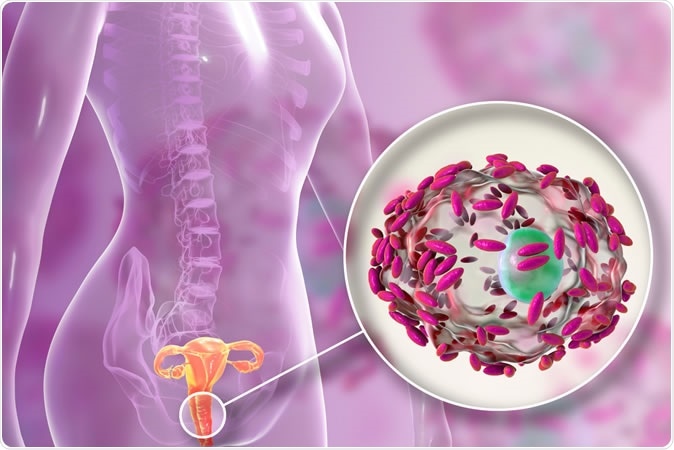
Bacterial Vaginosis/Vaginitis is used to describe various disorders that cause infection or inflammation of the vagina.
Bacterial Vaginosis/Vaginitis is the most common cause of vaginal symptoms among women. The prevalence in the United States is estimated to be 21.2 million (29.2%) among women ages 14–49, based on a nationally representative sample of women who participated in NHANES 2001–2004.
Women of any age, especially women of reproductive age and sexually active women, are particularly susceptible to bacterial vaginosis/vaginitis.
VAGINAL DISCHARGE
- One of the most common symptoms of Bacterial Vaginosis is the flow of a whitish, yellowish, or greenish discharge from the vagina of the female that may be a sign of infection.
-
The amount of vaginal discharge may increase during ovulation, before menstruation, during sexual arousal, and during pregnancy, taking birth control pills or wearing a uterine ring
-
Abnormal vaginal discharge usually turns yellow or green, looks like cheese or foam, smells, or even carries blood; causes may include infection, inflammation, cervix or genital tumors

CONSEQUENCES:
For many years BV not considered as sever disease.
Meanwhile is a situation which causes losses in working days and increases the cost of treatment [1].
Additionally increases the risk of …
- Infections of virus which affect the immune system[2].
- Sexual transmitted infections such as , gonorrhea , trichomoniasis , Herpes (HSV-2) [3, 4]
- Abortion, premature birth, after birth complications such postpartum endometriosis, pelvic inflammatory disease , preterm labour and preterm delivery and scars infections in pregnant [5--8].
- The possibility of HIV transmission [9,10].
1. Donders G. G. G., Vereecken A., Bosmans E., Dekeersmaecker A., Salembier G., Spitz B. Definition of a type of abnormal vaginal flora that is distinct from bacterial vaginosis: Aerobic vaginitis. BJOG: An International Journal of Obstetrics and Gynaecology. 2002;109(1):34–43. doi: 10.1111/j.1471-0528.2002.00432.x.
2. Myer L., Denny L., Telerant R., De Souza M., Wright T. C., Jr., Kuhn L. Bacterial vaginosis and susceptibility to HIV infection in South African women: A nested case-control study. Journal of Infectious Diseases. 2005;192(8):1372–1380. doi: 10.1086/462427.
3. Martin H. L., Jr., Richardson B. A., Nyange P. M., et al. Vaginal lactobacilli, microbial flora, and risk of human immunodeficiency virus type 1 and sexually transmitted disease acquisition. Journal of Infectious Diseases. 1999;180(6):1863–1868. doi: 10.1086/315127.
4. Cherpes T. L., Meyn L. A., Krohn M. A., Lurie J. G., Hillier S. L. Association between acquisition of herpes simplex virus type 2 in women and bacterial vaginosis. Clinical Infectious Diseases. 2003;37(3):319–325. doi: 10.1086/375819.
5. Hay P. E., Lamont R. F., Taylor-Robinson D., Morgan D. J., Ison C., Pearson J. Abnormal bacterial colonisation of the genital tract and subsequent preterm delivery and late miscarriage. BMJ. 1994;308(6924):p. 295. doi: 10.1136/bmj.308.6924.295.
6. Centers for Disease Control. Sexually transmitted diseases treatment guidelines 2006. MMWR. 2006;55(RR–11):50–54.
7. Minkoff H., Grunebaum A. N., Schwarz R. H., et al. Risk factors for prematurity and premature rupture of membranes: A prospective study of the vaginal flora in pregnancy. American Journal of Obstetrics and Gynecology. 1984;150(8):965–972. doi: 10.1016/0002-9378(84)90392-2.
8. Gravett M. G., Nelson H. P., Derouen T., Critchlow C., Eschenbach D. A., Holmes K. K. Independent Associations of Bacterial Vaginosis and Chlamydia trachomatis Infection With Adverse Pregnancy Outcome. JAMA: The Journal of the American Medical Association. 1986;256(14):1899–1903. doi: 10.1001/jama.1986.03380140069024. doi: 10.1001/jama.256.14.1899.
9. Cu-Uvin S., Hogan J. W., Caliendo A. M., Harwell J., Mayer K. H., Carpenter C. C. J. Association between bacterial vaginosis and expression of human immunodeficiency virus type 1 RNA in the female genital tract. Clinical Infectious Diseases. 2001;33(6):894–896. doi: 10.1086/322613.
10. Cohn J. A., Hashemi F. B., Camarca M., et al. HIV-inducing factor in cervicovaginal secretions is associated with bacterial vaginosis in HIV-1-infected women. Journal of Acquired Immune Deficiency Syndromes. 2005;39(3):340–346. doi: 10.1097/01.qai.0000146599.47925.e0.
CAN DOUCHING WITH WATER OR OTHER AGENTS HELP?
No, douching can increase the risk of getting bacterial vaginosis. The practice of washing or cleaning out the inside of the vagina with water or other cleansing agents alters the natural balance of the vagina and predisposes women to develop the condition. The vagina is self-cleaning, so douching is often not required.
Bacterial vaginosis, Causes, Signs and Symptoms, DIagnosis and Treatment. - YouTube 1:40
ARE ANTIBIOTICS USEFUL?

LADYBALANCE


LADYBALANCE increases vaginal Lactobacilli probiotics
- Return to normal defense system pH <4.5; most bacteria and fungi cannot survive
- No drug resistance and reduce alternative infections
- Can be used for pregnant women or breastfeeding
- Can be used to prevent BACTERIAL VAGINITIS
- Made in Denmark
- The world's first Prebiotic vaginal suppository
- Selling in Denmark and Europe for more than 15 years, safe and reliable
- According to a British study, nearly one thousand Ladybalance users have significantly improved all symptoms after one week of use.
